|
Winter arrived in full force to welcome in 2021 with snow blanketing the ground. And with snow, along came the excitement for sledding. While sledding can be a fun winter activity for children and adults alike, it is important to take some precautions to keep everyone safe.
1. Sled during daytime hours. Avoid sledding at night or in poorly lit areas to reduce the chance of injury. 2. Dress warmly. Hats, mittens/gloves and appropriate winter gear are advised to prevent hypothermia. Children are at a greater risk of hypothermia than adults. 3. Consider wearing a helmet. Yes, the American Academy of Pediatrics recommends considering a helmet, just as children do for skiing. Sledding can lead to concussions and other serious injuries. 4. Avoid sledding near trees, bodies of water and fences. 5. Young children should be supervised at all times. 6. Teach children how to roll off of a sled that will not come to a stop on its own. 7. Children should ride upright with feet first and in the forward -facing position. This will decrease the likelihood of a head injury. 8. Avoid pulling children on sleds behind vehicles. Have fun and enjoy the snow this winter! Dr. Jennifer Teegarden
0 Comments
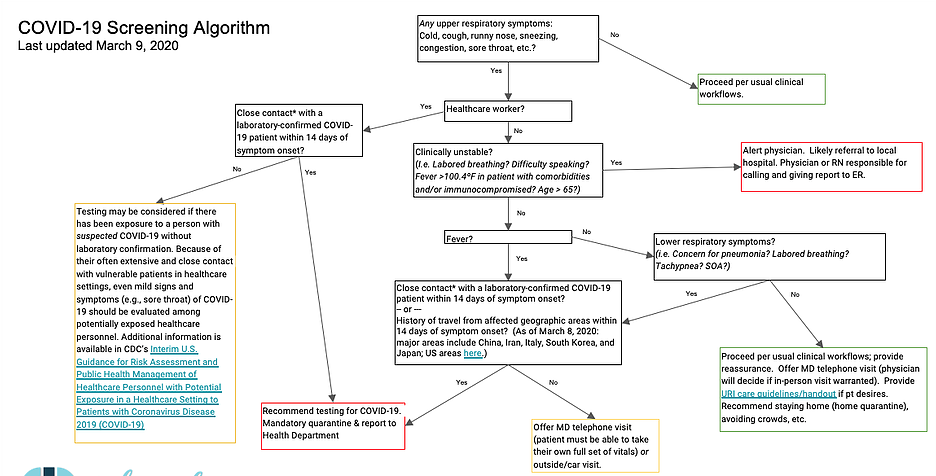
Many of our patients have asked about the novel coronavirus and we felt it necessary to address this directly. SARS-CoV-2 is the causative agent for the disease we now call COVID-19. In the past few months we have seen global spread of this virus and as of today there have been 423 total cases and 19 deaths in the United States. Currently, 35 states are reporting cases, including Kansas and Missouri. The closest case to our clinic has been a person in Johnson County who has recently been admitted to KU for observation and is doing well. This person was likely infected during a trip to the Northeast U.S. This being said, it is no longer a matter of WHETHER we will see this virus, but WHEN. We are committed to taking the best care of our patients possible during this time. For this reason, we are implementing guidelines to help keep ourselves and our patients as safe as possible as the situation develops. Here are some important highlights of our guidelines. You can find the complete algorithm below. Mild respiratory symptoms If you have a mild upper respiratory illness (cough, nasal congestion, and/or sore throat) we will ask you to stay at home and implement supportive measures (fluids, cough medicines, and rest). You should avoid public places (such as grocery stores or church functions) until you are feeling better and should wash your hands frequently. Consider staying in one room and bathroom in your house and disinfect these areas frequently, including doorknobs and light switches. Mild respiratory symptoms WITH fever >100.4ºF If you have respiratory symptoms such as cough, congestion, and/or sore throat and your temperature is OVER 100.4ºF, please call, text, or email our office so that we can set up a phone visit and determine if you need further care. If we determine that you need testing or need to be seen in the office. If an office visit is necessary, we may ask that you take extra precautions such as putting on a mask upon arrival or even having you call us on arrival if we feel it is safer to come evaluate you in the parking lot. Yes, in the parking lot. This is the safest way to prevent spread in our office and similar procedures are being implemented all over the country. The same guidelines apply regarding avoiding public places, washing your hands, and confining yourself to one area of your home to avoid infecting others. Severe respiratory symptoms WITH fever >100.4ºF AND significant shortness of breath If you are having respiratory symptoms, fever, and are feeling significantly short of breath or having trouble breathing, we will likely refer to the Emergency Room (ER) for further care. The most susceptible to this category of severe infection with COVID-19 are those over the age of 60 and those with underlying health conditions such as lung disease, heart failure, diabetes, or immunocompromised (patients taking steroids, biologic medications, or other immune suppressants, etc). Onset of severe symptoms tends to be around day 8-9 of infection. IF YOU HAVE TRAVELED TO HIGH RISK AREAS, INCLUDING DOMESTIC TRAVEL, IN THE LAST 2-3 WEEKS AND DEVELOP SYMPTOMS, YOU MAY NEED TO BE TESTED. PLEASE ALERT US BY PHONE OF ANY TRAVEL HISTORY OR POTENTIAL CONTACT WITH PATIENTS UNDER INVESTIGATION FOR COVID-19. FOR NOW, ALL TESTING WILL BE ARRANGED THROUGH THE JOHNSON COUNTY HEALTH DEPARTMENT AND NOT AT OUR OFFICE. REMINDERS ON FEVER
We cannot be more explicit than this: if we come into contact with someone who is positive for COVID-19, all Health Suite 110 staff who made contact with that individual will have to quarantine for 14 days. As we are a small practice, this may lead to a situation where we will have to close for all in-person interactions for up to (and potentially longer than) a 14-day period. If this were to occur, we would attempt to still offer telephone triage and telemedicine visits. We would like to prevent this if at all possible, so please help us do so by staying home if you are sick. We would be happy to write you a work note if needed. Again, we are putting these guidelines in place to prevent the spread of this illness to the most vulnerable around us. We appreciate your understanding, patience, and effort to keep everyone in our Health Suite 110 family healthy as we all see our routines altered by this virus. Please do not hesitate to ask questions or reach out. Sincerely, Your Health Suite 110 team Find out how you can protect yourself and your family HERE. Find out what to do if you are in a high risk category HERE. Find out how to mitigate spread in our community HERE. 3/14/20 UPDATE & ADDITIONAL COVID-19 RESOURCES As of 3/13/20, Johnson County has declared a state of emergency and the latest advisory from Kansas Department of Health and Environment reads: People should exercise vigilance when attending large public gatherings, particularly those people over age 60 and those with weakened immune systems or chronic medical conditions. If you have symptoms such as fever, cough or shortness of breath and believe you may have had contact with someone with a laboratory-confirmed case of COVID-19, stay home and call your health care provider. You may also call the KDHE phone bank at 1-866-534-3463 Monday through Friday, 8 a.m. to 5 p.m. Here are some websites we trust and would recommend looking into if you want more information: World Health Organization Center for Disease Control Kansas Department of Health and Environment For parents of young children 3/19/20 UPDATE
First, we would like to thank everyone for their support and encouragement as we work to navigate this evolving situation with you all. There are advances and updates coming in from around the world daily, sometimes hourly, and we are doing our best to stay up to date on the latest guidelines. With that in mind, we have a few updates. - In an effort to keep our clinic open and protect our staff and patients, we have reduced our in-clinic staff to 1 nurse and 1 physician while the rest of us work remotely. - ALL our physicians continue to be available by email and can arrange phone or in-person visits as necessary. - We will continue to reschedule all non-essential clinic visits during this time and appreciate everyone’s flexibility and patience. Medication refills: please continue to use our online refill request form or contact clinic directly at [email protected] or 913-948-7652. We do request at least a 48 hours notice for refill requests – thanks! a) Curbside pick-up - just call once you are parked at clinic and we’ll bring it out to your car (standard until further notice). b) Lockbox - located just outside clinic doors – you will be sent a code and can pick-up anytime during or after clinic hours. c) Mail delivery - about $12, may take up to 1 week after request. d) NEW Courier service (if unable to utilize above) - delivery to your doorstep in 1-2 days by kind volunteers. Tips appreciated! Call clinic for more details. General COVID-19 updates/reminders: - Mild upper respiratory infections can look like the common cold (cough, sore throat, fever) and should be treated at home. - Lower respiratory infections can result in pneumonia and cause cough, fever and shortness of breath. Severe symptoms may require hospitalization. - Seniors and those with chronic medical conditions are at the highest risk for developing severe symptoms. - Treatment is supportive as there are no currently approved treatments specifically for COVID-19. Some evidence that Zinc and certain antimalarial drugs (chloroquine, hydroxychloroquine) may be helpful. We are keeping a close eye on these developments. - Testing is not widely available at this time due to limited supplies of testing materials and personal protective equipment for clinicians outside of the hospital. Bottom line: everyone should be practicing social distancing during this time. Social distancing is putting space (at least 6 feet) between individuals to prevent the spread of illness. We encourage people to put this measure into practice for the health and safety of all. Community updates: - Jackson County has had their first cases and has prohibited groups of more than 10 through May 15, 2020. Jackson County updates. - Johnson County has now reached community transmission levels. Johnson County residents with mild symptoms should isolate at home and away from others for at least seven days after symptoms started or for 72 hours after fever is gone without the use of fever reducing medications and symptoms have significantly improved, whichever is longer. Anyone with more severe symptoms should call their healthcare provider. Individuals who have mild symptoms should not expect to be tested at this time. Kansas Health Department quarantine updates (including recent travel to Florida). Dr. Dana Hawkinson, infectious disease specialist at KU has good advice of what to do if you are feeling sick. In summary: 1. Don’t panic. 2. Stay at home and treat like any other virus with rest, fluids, pain/fever medications as needed. 3. If you have severe or worsening symptoms, contact your physician who can advise you on home treatment and if evaluation in the ER is necessary. We will continue to keep you posted with updates thank you for trusting us with your care. Health Suite 110 With spring break on the horizon, and summer just around the corner, many Americans will be planning and preparing for upcoming travels. Whether you are going on a road trip to visit family or traveling abroad, here are some tips to make sure you prepared for your journey.
1. Prescription medications: if you or your family members take prescription medications, it is important to make sure you have an adequate supply to last the duration of your trip. One or two weeks prior to your departure, check your prescription bottles and reach out to your doctor’s office if you are in need of a refill. If traveling by plane, be sure to pack your prescription medications in your carry – on bag, in the event your checked luggage were to be misplaced or lost. 2. Over-the-counter medications: you may consider packing some over-the-counter medications such as Ibuprofen, Tylenol, antibiotic ointment and band-aids. If you will be hiking or going on other outdoor adventures, bring a first aid kit along. 3. Health information: having a list of your medications, allergies, medical diagnoses and contact information for your physicians is advised when traveling. 4. Medical alert bracelets: if you typically wear a medical alert bracelet, be sure to not leave that behind at home. Wear it as you usually would. 5. Vaccines: if your vacation will be taking you abroad, be sure that you are up to date on the recommended vaccines. Visit www.cdc.gov and click the link for “travelers health” for a list of what vaccines are advised depending on what country you will be visiting. Ask your doctor about any vaccine questions and for information on where you can receive those vaccines. If you need vaccines, plan to receive those at least two weeks prior to your departure. 6. Health insurance: if you have health insurance, be sure to bring your wallet card along. 7. Sunscreen: protect your skin. Sunscreen does have an expiration date, so make sure yours is in date before you lather up. 8. Cold weather destinations: if you will be hitting the ski slopes or venturing to other destinations with extreme cold, be sure to pack all of your winter gear. Wear layers, have appropriate gloves, hats, etc. Be aware of the temperatures and amount of time outdoors to prevent frostbite and other injuries that can occur with prolonged exposure to extreme cold. 9. Hydrate and healthy foods: traveling can mean long days, long flights and long car rides. Be sure to stay hydrated and eat healthy foods. Eating healthy can help to support your immune system and keep you feeling good during your travels. 10. Have fun: we hope your time away from home is a chance to laugh, have fun and make some great memories! If you have any other travel questions, be sure to check in with your primary care physician! Dr. Jennifer Teegarden If you have a teenager at home, you likely know all too well about sleepy teens. Teenagers need on average about 9 to 10 hrs of sleep at night, but most of them aren’t getting this amount of rest consistently. Teenagers are growing, not just physically, but their brains are also developing, increasing their need for more sleep.
So, why are they not getting the recommended amount of sleep? Well, most teens brains are engineered to want to stay up late and sleep in. However, most middle schools and high schools start early, with most teens arriving to school each morning by 8 am and some as early as 7 am. This translates into early wake times. Sports, late evening practices, extra – curricular activities and increased amounts of homework often mean late nights for many teens. Lack of sleep or sleep deprivation in teens can have significant consequence and affect them in a variety of ways. Teens lacking in sleep may often be more moody or irritable. Parents may also notice an increase in more risk – taking behaviors such as fast driving, smoking, and drinking alcohol with chronic sleep deprivation. There has also been an association between lack of sleep and an increase in reported car accidents and teens falling asleep at the wheel. School performance often suffers as well and should be a red flag if parents are noticing a change in their teen’s grades. Attention, memory, and decision making all are affected by not getting enough zzz’s. So, if this sounds all too familiar with your teen, what can you do to help? Well, there are a number of actions parents can take to help their teens get the rest they need. 1. Sleep schedule: yes, teens can benefit from a sleep schedule. Having a nightly routine and sticking to it. A consistent bedtime and wake time can help. 2. Avoid oversleeping: (insert teen eyeroll). Sleeping in might just be your teen’s favorite weekend pastime. However, sleeping in until noon on Sundays is going to make it difficult to get to bed on time Sunday evening. 3. Early afternoon naps: If your teen is tired after school and he or she has time to nap before their evening practice or activity, a 30 minute nap can help provide some much needed rest. 4. Avoid screens: now, this is a hard one. Avoiding use of TV’s, smart phones and other screens at least 1 hour prior to bedtime is advised. 5. Avoid caffeine: teens should have limited caffeine consumption. Avoiding all caffeine during the afternoon and evening hours can help as well. If your teen is persistently tired despite implementing some actions to increase their rest, or you notice excessive snoring, contact their primary care physician for further evaluation and recommendations. Sweet dreams! Dr. Jennifer Teegarden Patient: Hey doc, thanks for all your great care, but I have insurance now so need to cancel my membership.
Me: Sorry to hear you are leaving. Best of luck! Remember, we care for folks regardless of their insurance status and most of our patients HAVE insurance, so no reason to quit if you prefer to remain a member. Patient: Ok, thanks. I really hate to leave, but don’t see the point of paying for membership when I have insurance. Will miss you all! 1 month later Patient: Hey doc, I really need to get in for [insert any medical need], but I can’t find a primary care physician who’s accepting patients within the next 6 months. Do you have any recommendations? Me: Not anymore. --- Recently I got the news that another Family Medicine colleague was leaving primary care due to the misery that is traditional practice. Even her private practice setting couldn’t protect her from the outside forces that threaten the sanctity of the patient-doctor relationship. As is often the case, this physician was finally fed up with the bureaucracy, the endless check-boxes, the pressure to see more patients in less time and the drain on her personal and professional satisfaction in a career she worked so hard to achieve. And I don’t blame her one bit. Healthcare, especially PRIMARY CARE is based on relationships. This means that doctors are not interchangeable cogs in a machine and that seeing “someone” is not the same as seeing YOUR physician who knows you, your preference, quirks and life circumstances through a relationship that is established over years together. There is nothing that can replace the value of being known – especially as this also helps to prevent misdiagnosis, over-testing and over-treatment and their downstream effects. In fact, studies continue to show that states with more primary care physicians are healthier and live longer, even when socioeconomic and lifestyle factors are taken into account. Unfortunately, despite the proven effectiveness and overall cost-savings, primary care is undervalued in this country and many physicians have abandoned what used to be a fulfilling career. What has driven us to this point? Arguably, one of the biggest drivers in our current healthcare crisis is Our Unhealthy Addiction to Health Insurance, which is summarized beautifully by one of our DPC colleagues, Dr. Jeffrey Gold. As Dr. Gold reminds us, “The main mistake that we have succumbed to as a society is that we have deviated from the original intent of health insurance. The true purpose of health insurance was to protect people against financial ruin in the event of an unexpected, major occurrence – just like car insurance, life insurance, and homeowner’s insurance. But things got murky when people were indoctrinated into the belief that good health insurance should “cover everything” because “everything in healthcare is expensive.” Not only has the reliance on insurance resulted in an immoral spiraling of inflated pricing, more unnecessary testing, referrals and aggressive treatments, but it has also convinced people that TIME spent listening to patients and TIME to do a thorough physical exam is not worth paying for. All of this had led to people forgetting that health insurance…is NOT…health care. Think about that for a moment. Health insurance is a product that helps protect against financial ruin in case of unexpected, expensive, catastrophic events. Health insurance companies are for-profit entities that are in the business of making money. Health care is what you need when you are sick or injured. Health care is provided by medical professionals (doctors, nurses, etc) who have spend many years in continual training and are in the business of helping people. While both are necessary (after all, home-owners insurance is certainly important in case of a fire), only one actually provides the care. Hint: it’s not the insurance company. So, if personalized health CARE provided by a doctor who knows you and will be there for you regardless of your health, age, income, insurance or job-status is important to you, then invest in a Direct Primary Care practice. If supporting doctors who are willing to sacrifice their financial stability in order to provide real care to patients again, then invest in Direct Primary Care. If transparency in pricing and reducing unnecessary testing and treatment is important to you, then invest in Direct Primary Care. I could go on and on, but instead, I’ll leave you with one of my favorite Margaret Mead quotes. “Never doubt that a small group of thoughtful, committed, citizens can change the world. Indeed, it is the only thing that ever has.” To your health! Dr. Vannaman There has been a lot in the news recently about voluntary recalls of Zantac (ranitidine). In short, the FDA found trace amounts of N-nitrosodimethylamine (NDMA), a probable carcinogen (cancer-causing compound), in some lots of the medication by several manufacturers.
While the headlines are scary, this topic deserves a little unpacking. First, let’s gain a little perspective. According to the FDA, the levels of NDMA in many tested ranitidine products are similar to those consumed through "common foods like grilled or smoked meats.” For some people, this statement is quite reassuring, while others are thinking, “What?! My favorite grilled meat can cause cancer?”. Well, yes and no. Cancer is caused when damages to DNA result in uncontrolled over-growth of a cell or tissue. Most of the time, our cells recognize the damage and either fixes the DNA or destroys the cells that have gone rogue. A person’s overall risk of cancer is based on a number of factors including genetics and environment exposures https://www.cancer.gov/about-cancer/causes-prevention/risk/substances. While some exposures can be avoided (tobacco smoke, excessive sun exposure), others are more difficult to avoid since they are present in the environment, including the air we breathe and the food we eat. Health Suite 110’s stock of ranitidine was not affected by these recalls as we are stocked by a different manufacturer. That said, the FDA recommends “patients taking prescription ranitidine who wish to stop should talk to their health care professional about other treatment options. Consumers taking OTC ranitidine, which is used to prevent and relieve heartburn associated with acid indigestion and sour stomach, may consider using other OTC products approved for their condition. FDA’s testing of samples of alternatives such as Pepcid (famotidine), Tagamet (cimetidine), Nexium (esomeprazole), Prevacid (lansoprazole), and Prilosec (omeprazole) show no NDMA in these medicines”. You can read more about the recall and specific lots affected on the FDA website: https://www.fda.gov/drugs/drug-safety-and-availability/fda-updates-and-press-announcements-ndma-zantac-ranitidine. For patients who prefer to switch from taking Zantac, these medications are not all interchangeable. While Zantac, Pepcid and Tagament are all histamine-blockers (H2-blockers), things like Prevacid and Prilosec are proton-pump inhibitors (PPIs) and have different implications. H2-blockers are generally felt to be safe for long-term use, while long-term use of PPIs can increase the risk for C.diff, pneumonia and osteoporosis. If you require antacid medication on a daily basis, be sure to discuss with your physician. Sometimes there is an underlying cause that can be treated (H. pylori infection, obesity, food triggers) and other times the risk of taking a medication long term far outweighs the risks of not taking it, particularly for folks who have pre-cancerous changes in their esophagus from long term reflux (Barrett’s esophagitis). In summary:
Five Steps for Cancer-Safe Grilling 1. Marinate: Studies suggest that marinating meat before grilling can decrease formation of carcinogens. 2. Pre-Cook: If you are grilling larger cuts, you can reduce the time your meat is exposed to flame by partially cooking it in a microwave, oven or stove first. 3. Go Lean: Trimming the fat off your meat can reduce flare-ups and charring. Cook your meat in the center of the grill and make sure to flip frequently. 4. Mix It Up: Cutting meat into smaller portions and mixing them with vegetables can shorten cooking time. 5. Go Green: Grilling of vegetables and fruits produces no carcinogens. So, add veggies and cut down the amount of meats. Happy grilling! Kylie Vannaman MD For some, the holidays are a time for gathering, joy, cheer, family, friends, peace and togetherness. For others, the holidays are instead filled with isolation, stress, depression, family turmoil, heartache, and loneliness. And maybe for the majority of us, it is a combination of the above.
During this season of thanksgiving, it can sometimes be difficult to maintain an attitude of gratitude. Some may feel it is only obtainable when all is going well. According to Robert A. Emmons, Ph.D (noted to be the world’s leading scientific expert on gratitude and a professor of psychology at the University of California, Davis, and the founding editor-in-chief of The Journal of Positive Psychology), one of the five myths about gratitude is that it isn’t possible or appropriate in the midst of adversity or suffering. “Some argue that it’s impossible to be grateful in the midst of suffering. When life is going well, when there’s abundance—sure, then we can be grateful. But what about when we’re facing hard times? I believe not only is gratitude possible in those circumstances—it’s vital to helping us get through them. When faced with adversity, gratitude helps us see the big picture and not feel overwhelmed by the setbacks we’re facing in the moment. And as I’ve suggested above, that attitude of gratitude can actually motivate us to tackle the challenges before us. Without a doubt, it can be hard to take this grateful perspective, but research suggests it is possible, and it is worth it.” https://greatergood.berkeley.edu/profile/robert_emmons#articles Gratitude has been studied in patients after heart attacks. Gratitude at 2 weeks after a heart attack was associated with a higher self-reported adherence to medical recommendations (diet, exercise, medication adherence, stress reduction) and improved emotional well-being 6 months later. It was concluded that gratitude may help recovery from a heart attack and that interventions promoting this positive construct could help improve adherence and well-being. https://www.ncbi.nlm.nih.gov/pubmed/27796252 In another study of asymptomatic heart failure patients, gratitude journaling decreased lab results related to heart failure morbidity such as inflammation. https://www.ncbi.nlm.nih.gov/pubmed/27187845 Here is a TED talk I recently watched which involves a physician and her journey with gratitude while caring for a son with an incurable and terminal illness. Can you apply her experience to your own life’s situations? - https://www.youtube.com/watch?v=HHTmiHB6aXk&feature=youtu.be&list=PL9wE6J5iLNROCZYibeUCT9vWStvOc6EOZhttp%3A%2F%2Fyoutu.be%2FHHTmiHB6aXk%3Flist%3DPL9wE6J5iLNROCZYibeUCT9vWStvOc6EOZ But how can I develop more gratitude? I recommend a review of the following article by Dr. Emmons titled 10 Ways to Become More Grateful - https://greatergood.berkeley.edu/article/item/ten_ways_to_become_more_grateful1 Lastly, how can I be better prepared for the upcoming holiday season (and any “season” of life)? I often recommend guided imagery, which is a form of meditation, as a way to practice mindfulness. By reconnecting with ourselves and being present for a short period of time, we can be better prepared for the stressors and challenges of life. To see if guided imagery is right for you, try listening to guided imagery audio for free on this Kaiser Permanente website - https://healthy.kaiserpermanente.org/health/care/!ut/p/a0/FchBDoMgEADAt_iAzYZEYfFmhH6hhdsGiZIIGELt99seZ9DjC33hO-3cUy18_uxCLD22md9bqnCnLVZ8okd_Nd4zoysVAocj_o9bT-GM6IzVap2MBamlBCGsgEWPBohoUkKp8UErXjnTZxmGL2IKPpI!/ If you find these audio sessions helpful and would like more, I recommend resources from the following website - https://www.healthjourneys.com “Gratitude unlocks the fullness of life. It turns what we have into enough, and more. It turns denial into acceptance, chaos to order, confusion to clarity. It can turn a meal into a feast, a house into a home, a stranger into a friend. It turns problems into gifts, failures into successes, the unexpected into perfect timing, and mistakes into important events. It can turn an existence into a real life, and disconnected situations into important and beneficial lessons. Gratitude makes sense of our past, brings peace for today, and creates a vision for tomorrow. Gratitude makes things right.” Melody Beattie Dr. Charles Willnauer We usually think of “dementia” as simply memory loss, but it is much more than that. The term “dementia” is defined as having memory loss AND difficulty in one other area such as:
These symptoms must interfere with independence and quality of life to be considered to be consistent with dementia. What causes this horrible disease? There are several diseases that affect the brain which can result in dementia.
What tests should you have? The first step is to have a conversation with your primary care doctor. There are a few blood tests you might discuss, like thyroid levels, B12, and other blood tests. Imaging may include CT or MRI brain. There are various other experimental imaging studies that are under investigation. Finally, a lumbar puncture might be needed as well to analyze the spinal fluid. Again, the best place to start is with talking with your primary care doctor. How can you treat this disease? It all depends on the type of disease. There are a few medications that may help with quality of life and memory. Unfortunately, there are no treatments that can halt the progression of the disease. Clinical trials help us find a cure and current trials are testing medications that block the progression of the disease. To decrease the risk of developing dementia, follow a healthy dose of physical activity, a healthy diet, and engage in social interaction. As simple as this may sound, these 3 recommendations can be difficult to complete consistently. Genetics may also play a role in developing dementia. Unfortunately, there are no genetic tests that are validated that accurately predict the development of dementia. Cherish each and every moment. Live with gratitude. Dr. Ahmed September is PAD awareness month.
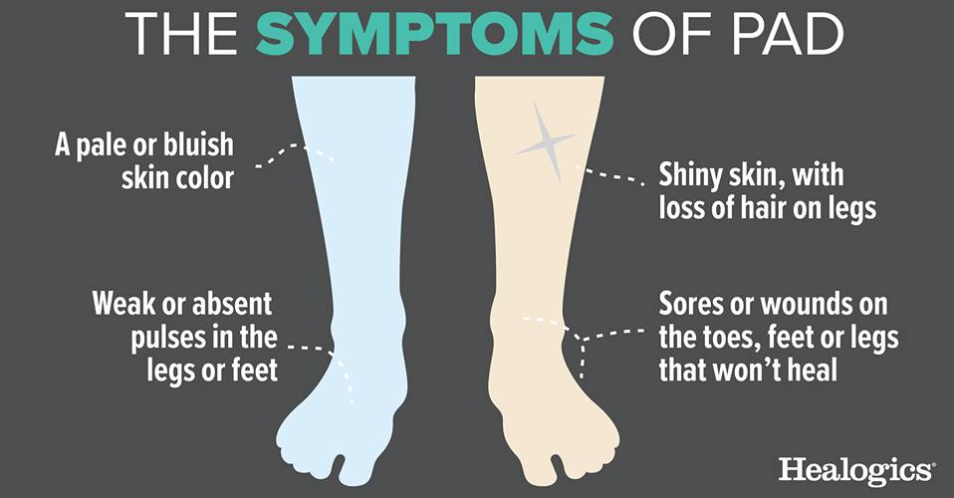
What is PAD? Peripheral arterial disease is a chronic, life threatening condition of the the circulatory system. It may also be referred to as claudication, poor circulation or vascular disease and it affects up to 20 million Americans. The cause of PAD is the blockage or narrowing of the blood vessels that transport blood from the heart to the lower extremities or legs. This blockage or narrowing is due to atherosclerosis or the build-up of plaque. Complications of PAD include sores and wounds that if left untreated can result in limb amputation. So, who is at risk for PAD? There are a number of potential risks factors that all patients should be aware of. Those include: - Smoking - High blood pressure - Diabetes - High cholesterol - Obesity - Age > 60 - Family history of vascular disease PAD can present with a number of different symptoms. Common symptoms that patients experience include: - Leg pain when walking - Cramping or pain in the leg muscles brought on with increased physical activity - Weakness or numbness in the legs - The legs or feet feeling cold - A change in color of the legs - Sores on the legs or feet that do not heal A healthy lifestyle can help to reduce the likelihood of not developing peripheral arterial disease. Avoiding smoking, increasing exercise and physical activity and eating a diet of nutritious foods can all help to reduce risk. If you have risk factors for PAD or are experiencing symptoms which could be due to undiagnosed peripheral arterial disease, please reach out to your primary care physician. Patients may also visit the American Heart Association at www.heart.org for additional resources and information. Dr. Jennifer Teegarden School is back in session and in addition to hitting the books, many students are back in the gym training for fall sports. Each year, more than 60 million school aged children participate in organized sports! Being a member of a sports team can bring a number of great experiences and life lessons for students, along with fun and great memories. So whether your daughter or son plays volleyball, basketball, football, tennis, baseball, runs track or is a tumbling gymnast, it is important for parents and students to be aware of overuse injuries.
What is an overuse injury? An overuse injury is damage to a bone, muscle, tendon or ligament caused by repetitive stress and without given the time to properly heal. Children and teens are at increased risk for overuse injuries for a multitude of reasons. Their growing bones are more susceptible to injury and they might not always be aware the symptoms that they are experiencing could be an overuse injury. Some common examples include tennis elbow, runner’s knee, pitcher’s elbow and shin splints. What symptoms should student athletes and their parents be looking for? Well, there are four stages of overuse injuries and how they typically present and progress. Stage 1: Pain in an affected area after activity Stage 2: Pain in an affected area with activity, but not limiting performance Stage 3: Pain during activity and limiting performance Stage 4: Chronic persistent pain even at rest What can student athletes and parents do to help prevent overuse injuries . . . 1. Every student athlete should have a PPE or preparticipation physical evaluation. Ideally this evaluation or sports physical should be performed by your child’s primary care physician, who has knowledge of their prior health history and can follow them for any chronic conditions as well as help manage any acute injuries. 2. All student athletes should maintain year-round fitness, during the season and the off season as well. 3. Proper warm ups and cool downs with all practices and games. 4. Limit a particular sport to 5 days per week. This also helps to prevent burnout. 5. It is recommended that athletes participate in only one sport and on only one team each season. 6. Encourage participation in a variety of sports. This gives your child an opportunity to learn new skills, make new friends and even maybe find a new passion. If your student athlete has pain or symptoms of concern, contact their primary care physician for an evaluation. We wish all of our student athletes a fun, safe and healthy season! Dr. Jennifer Teegarden |
Archives
January 2021
Categories
All
|
|
Clinic Hours
Monday-Thursday 9am-5pm Friday 9am - 12pm Closed for lunch 12-1pm daily CONTACT US!
7199 W 98th Terrace, Suite 110 Overland Park, KS 66212 Bldg #3 in Windmill Village phone:: 913-948-7652 fax: 913-273-2474 [email protected] |
Physician office hours:
Dr. Groves: Mon, Wed, Thurs 9am-5pm, Tues & Fri 9am-12pm Dr. Teegarden: Mon-Wed 9am-5pm. Thurs & Fri 9am-12pm Dr. Vannaman: Mon, Tues, Thurs 9am-5pm. Wed & Fri 9am-12pm Dr. Willnauer: Mon-Thurs 9am-5pm & Fri 9am-12pm |
2024 Holidays - Clinic CLOSED
New Year's Day - Jan 1 MLK Day - Jan 15 President's Day - Feb 19 Memorial Day - May 27 Annual staff retreat - June 13-14 Juneteenth - June 19 Independence Day - July 4, 5 Labor Day - Sept 2 Veteran's Day - Nov 11 Thanksgiving - Nov 28, 29 Christmas - Dec 24, 25, 26 |









 RSS Feed
RSS Feed